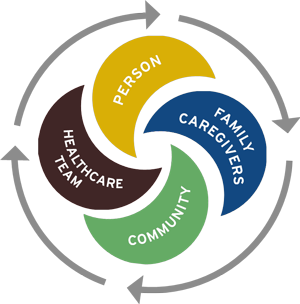
Care Coordination & Integration
In order to have an effective healthcare system that is patient centered, care coordination is inherent. This involves significant communication between health professionals, to ensure that quality care is consistently provided to patients. In addition, as care teams strive to make primary care the center for all of a patient’s general needs, further integration may be necessary. With primary care serving as the “hub” for most patients, incorporating facets of other fields is not only plausible but an obvious next step for better coordination.
The PCC has consistently acknowledged the need for an increase in care coordination, and further integration of other fields, such as oral health and behavioral health. The PCC has shown a commitment to further primary care integration by creating the Primary Care and Behavioral Health Integration Workgroup and participating in grants centered around increasing the visibility of oral health in the primary care space.
Resources

Brown & Toland Physicians | September 2014

Annals of Family Medicine | September 2014

Centers for Medicare & Medicaid Services | September 2014
Hospital Topics | September 2014

The Commonwealth Fund | August 2014

Aligning Payers and Practices to Transform Primary Care: A Report from the Multi-State Collaborative
Milbank Memorial Fund | August 2014
- ‹ previous
- 12 of 34
- next ›
News
March 1, 2019 | Washington Post
February 27, 2019 | Family Medicine
- ‹ previous
- 12 of 90
- next ›
Events & Media
December 4, 2018 | Health Affairs
November 27, 2018 | SCIO Health Analytics
December 3, 2018 | Berkeley Research Group, LLC
- ‹ previous
- 12 of 72
- next ›
Related Content
Pages
|
Title |
Source | Date |
|---|---|---|
| Demand grows for care coordinators in primary care | Modern Healthcare | March 28, 2015 |
| Demystifying and strengthening integrated care | National Association of Primary Care | April 30, 2018 |
| Designing Care Models to Treat High-Need, High-Cost Patients | RevCycle Intelligence | July 12, 2017 |
| Direct primary care: The key to cost savings and improved health? | Benefits Pro | May 20, 2019 |
| Discussing Barriers to Closing the Behavioral Health Integration Gap | Psychiatry Advisor | July 1, 2019 |
| Disinvesting In Primary Care? | Health Affairs | March 14, 2018 |
| District will no longer guarantee ambulance rides for nonserious patients | Washington Post | March 1, 2019 |
| Docs, Nurses Press for Changes to MACRA Rule | MedPage Today | June 27, 2016 |
| Doctors and Nurses, Not Learning Together | New York Times Well Blog | April 30, 2015 |
| Doctors Can Bill Pharmacist Services 'Incident-To,' CMS Says | Medscape | June 19, 2014 |
Pages
Associated Stakeholders:
Secondary menu
Copyright © 2024 Primary Care Collaborative